Table of Contents
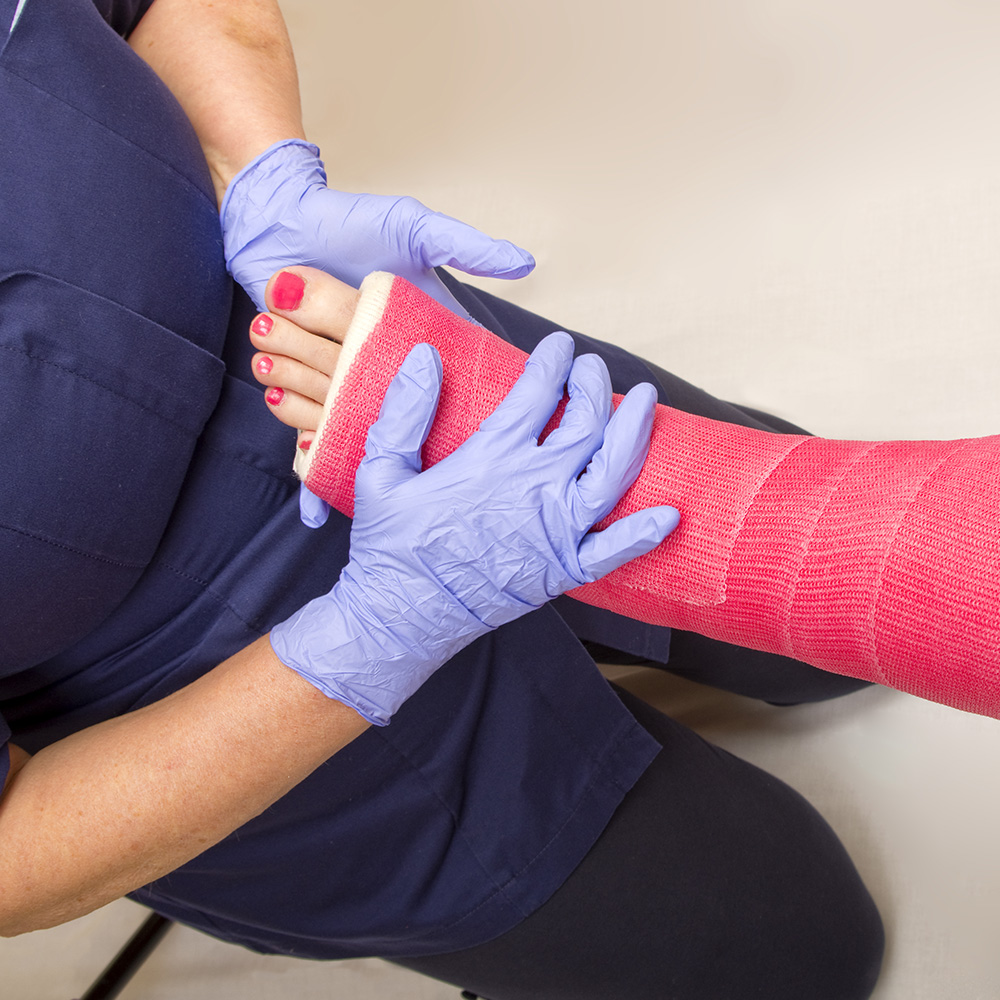 Many of us associate broken bones with a traditional plaster cast–the kind our friends would sign in grade school. But casts–and other treatments for arm and leg injuries– have changed over the years. For many fractures, casts still play a crucial role in the healing process. But for other injuries, orthopaedists are now opting for removable modern splints and boots that offer greater comfort and flexibility. The American Academy of Orthopaedic Surgeons says the treatment of broken bones follows one basic rule: “the broken pieces must be put back into position and prevented from moving out of place until they are healed.” Whether a cast is needed depends on the patient, what kind of injury you have and how your doctor approaches the process.
Many of us associate broken bones with a traditional plaster cast–the kind our friends would sign in grade school. But casts–and other treatments for arm and leg injuries– have changed over the years. For many fractures, casts still play a crucial role in the healing process. But for other injuries, orthopaedists are now opting for removable modern splints and boots that offer greater comfort and flexibility. The American Academy of Orthopaedic Surgeons says the treatment of broken bones follows one basic rule: “the broken pieces must be put back into position and prevented from moving out of place until they are healed.” Whether a cast is needed depends on the patient, what kind of injury you have and how your doctor approaches the process.
What Are Different Types of Casts?
Sometimes a patient needs the ongoing structured support of a cast to keep an injured limb immobilized for weeks or even months. A cast features soft padding under a rigid surface, usually plaster or fiberglass.
- Plaster casts resemble the traditional casts many of us are familiar with from our childhoods. They’re less expensive and easier to mold than newer materials and offer a precise fit that’s needed for some injuries. However, they’re usually heavier than fiberglass and can irritate the skin. They can’t get wet and need to be wrapped in plastic for bathing.
- Today’s colorful, high-tech fiberglass casts function in much the same way as plaster. However, they’re more breathable and less likely to irritate the skin. They’re also lighter and more porous than plaster so that x-rays can be taken with the cast on. Fiberglass casts can also be waterproofed by using a special liner, making bathing and other activities easier. If they get wet, drying with a blowdryer is an option.
What Are Some Concerns About Casts?
Along with the general discomfort that wearing a cast for six weeks can bring, medical concerns about rigid casts can arise.
- Compartment syndrome is one of the primary concerns with rigid casts. It occurs when a cast is put on before swelling subsides. It can cause pressure to build up and damage the muscles, nerves or blood vessels in the affected area.
- Casts can cause pressure sores and skin irritations.
- A 2018 British study suggests that immobilization in a cast can cause muscle atrophy, deep vein thrombosis and joint stiffness in older adults.
What Are Alternatives to Casts?
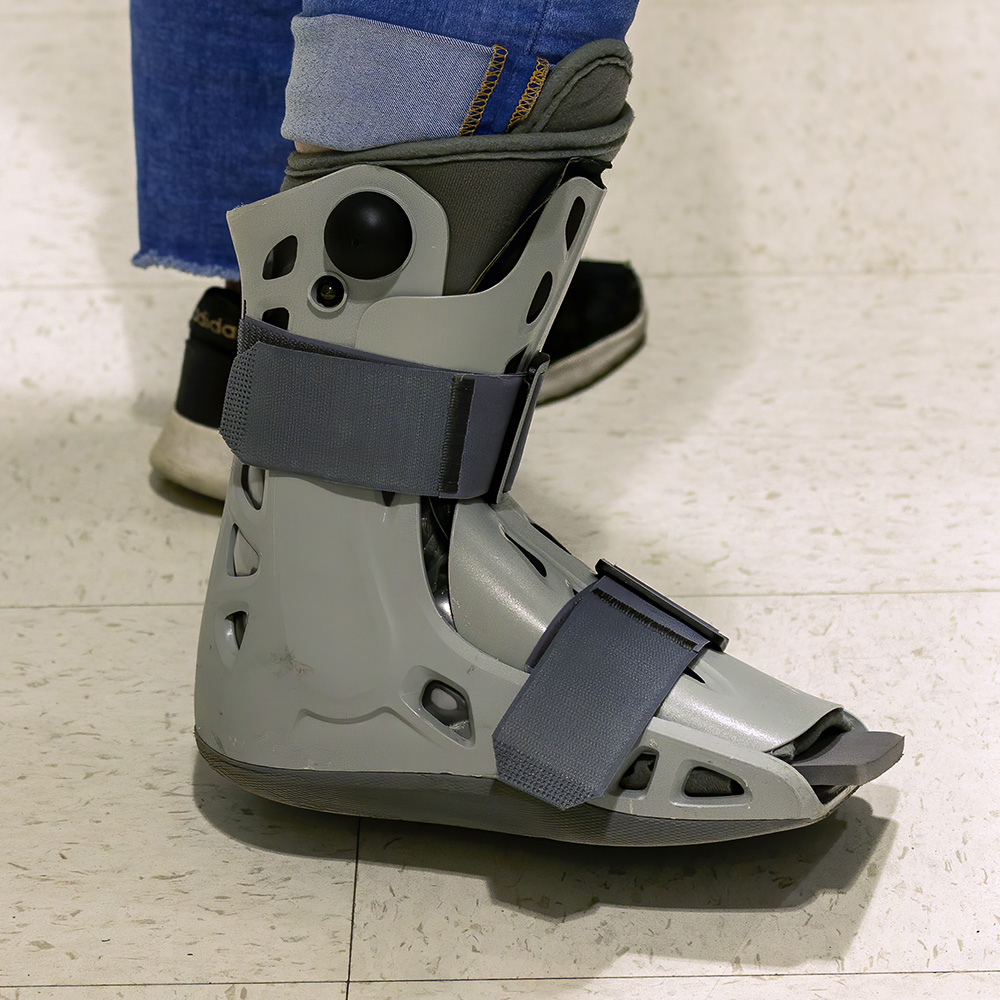 More and more, we’re seeing removable splints and walking boots as an alternative to casts–or used before or after a cast is put in place. While these options aren’t a solution for all fractures, they work well for some patients and injuries. In general, splints provide less support but more flexibility than a rigid cast. They’re easy to take on and off and allow your doctor to reevaluate your injury with x-rays or other diagnostic tools. They also tend to be more comfortable for patients.
More and more, we’re seeing removable splints and walking boots as an alternative to casts–or used before or after a cast is put in place. While these options aren’t a solution for all fractures, they work well for some patients and injuries. In general, splints provide less support but more flexibility than a rigid cast. They’re easy to take on and off and allow your doctor to reevaluate your injury with x-rays or other diagnostic tools. They also tend to be more comfortable for patients.
Several recent studies have shown that removable splints are just as effective and more comfortable and convenient for treating some common wrist and forearm injuries in children. Prefabricated splints are becoming the preferred treatment for partial “buckle” fractures in children.
Splints can also be a preferred treatment for sprains, some fractures, joint dislocations and soft tissue injuries in adults. Removable boots are often an alternative for minor fractures and sprains to the foot or ankle. Boots can also provide support after a cast is removed.
Casts, Splints, or Both? Ask Your Orthopaedist
According to AAOS, how your orthopaedist immobilizes an injured bone depends on:
- Location of the fracture
- Nature of the fracture
- Patient’s age and activity level
- Surgeon’s preferences
Your orthopaedist will take all of these factors into consideration when deciding which approach is best. Often, using both a cast and a splint or boot can optimize the healing process. Your surgeon may start with a splint and then move to a cast after the swelling subsides. Patients may use a rigid cast for several weeks and then go back to a splint for additional stability during the final weeks of healing. As you navigate the new landscape of rigid casts and removable splints, it’s essential to work with an orthopaedic surgeon you trust to make the right call. At Countryside Orthopaedics, we’ve watched technology and materials evolve throughout our decades in practice. We embrace new approaches and technology. However, it’s not about trends but about treatments that will help our patients heal quickly and completely. Every patient, every injury and every path to healing are different, and our recommendations are always tailored to your individual needs.